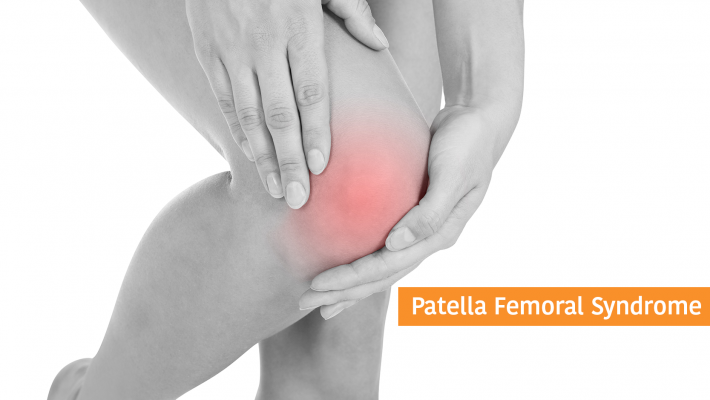
One of the most common knee problems that I see in clinic is Patella Femoral syndrome; also sometimes know as runner’s knee.
The problem causes pain in the front central portion of the knee usually worse when running or walking up or down hill or going up and down stairs (down particularly). Often there can be pain when sitting with knees bent, which is why the condition is also known as theatre goers knee. Pain comes from behind the kneecap (Patella) where it contacts with the thigh bone (femur).
Prolonged excessive shearing forces between the back of the patella and the front of the femur as the patella no longer tracks nicely between the groves formed by the bottom of the femur.
The problem is usually caused by biomechanical dysfunction, over pull of the lateral quadriceps, excessive pronation or supnation (rolling in or rolling out) of the foot. Overuse in sports or activities which are tough on the knee can also lead to patella femoral syndrome, running, jumping, cycling often exacerbated by biomechanical problems.
This results in inflammation, pain and eventually thinning and softening (Chondromalacia) of the articular cartilage behind the patella and on the femur. The condition can also be secondary to fractures, Osteoarthritis and bony tumours, i.e. changes in the bony structure of the knee.
The problem is usually diagnosed on examination and history, although X-ray and MRI can be useful if the diagnosis is not straightforward.
Treatment can involve any or all of the following, controlling excessive biomechanical dysfunction (pronation or supination) of the feet and legs with either strapping or orthotics, quadriceps strengthening, stretching of posterior muscles of the leg and thigh, and sometimes direct treatment to the knee, laser, icing and anti-inflammatory drugs.
Treatment will depend on the severity and duration of the problem and identification of the underlying causes. Prognosis is full recovery, and a return to normal activities once underlying causes are identified and addressed. I think podiatrists are in a unique position the treat this problem as we are able to address the underlying biomechanical problems to resolve the condition. But then I am a bit biased!
Philip Mann Podiatrist/Chiropodist tel: 686 912 307 or www.footpodiatrist.com