Achilles tendonitis
This condition presents with pain at the back of the ankle, base of the calf muscle, inflammation of the tendon and or tendon sheath. Often worse on rising in the morning and walking up hills or running.
Treatment may involve any or all of the following stretching, foot ware changes, orthotics, and Laser treatment.
Arthritis
The two most common types of arthritis that affect the foot are Osteoarthritis and Rheumatoid arthritis.
Osteoarthritis is degeneration of the joint usually involving swelling of the affected joint. It can affect single or multiple joints. There is often associated pain and weakness. This is basically the wear and tear disease, the swelling is partly soft tissue and synovial fluid and partly bone as the joint tries to remodel and repair its self. The disease can manifest its self in any joint of the foot.
Rheumatoid Arthritis is a systemic auto immune disease affecting all connective tissue particularly but not limited to joints. There is pain swelling and muscle weakness of multiple joints often with nodular involvement. Bony changes often lead to misalignment and even partial dislocation of joints. In the foot the first joint to be seen in is usually the great toe often over riding or under riding the lesser toes as the disease progresses, it can lead to sever corns and even ulcers.
Both diseases respond well to anti inflammatory drugs at the onset rheumatoid patients often require immunosuppressive drugs as the disease progresses. From a podiatry perspective treatments aim at pain reduction by treating corns’ ulcers, use of insoles and orthotics is often indicated to redistribute pressure away from joints. Low Level or cold Laser very good at settling down acute arthritic flair ups.
Bunions
Bunions are a form of arthritis of the 1st toe joint usually involving swelling and medial deviation of the first toe. This can be from either Osteoarthritis or Rheumatoid arthritis. There may be pain and inflammation.
Treatment may involve any or all of the following, foot ware advice, anti-inflammatory drugs, manipulation, orthotics, Laser, deflective padding and in severe cases even referral for surgery.
Bursitis
A Bursa is a small sack filled with synovial fluid usually there to protect a structure, for example there is a bursa between the Achilles tendon and the heel bone to prevent the tendon rubbing on the bone. There are two types of Bursa, anatomical (the ones we are born with and adventitious the type we develop to protect a certain area. Bursitis is inflammation of a Bursa.
Treatment may involve ant-inflammatory drugs, deflective padding, simple insoles or Laser.
Callous
Thickening of skin often but not limited to the underside of the foot (plantar surface) usually due to increased pressure or friction in that area often exacerbated by dryness. Can be painful and in severe cases usually associated with diabetes can result in ulceration.
Treatment involves sharp debridement (cutting off the callous) this is a painless procedure. The use of emollients is also beneficial.
Corns
A concentration of callous or hard skin over a bony prominence the area can be acutely painful and inflamed and if neglected, may even ulcerate. Treatment involves enucleating the corn (cutting it out) this is a painless procedure. Then reducing the pressure which originally caused it, by altering foot ware or deflective padding or simple insoles.
Capsulitis
Inflammation of the capsule of the joint usually associated with acute trauma (sports injury or over use) the area becomes hot swollen and painful.
Treatment may include anti-inflammatory drugs, reduction of trauma to area by rest and or biomechanical assessment and orthotic therapy.
Diabetes
Is increase in circulating blood sugar levels, there are two types of Diabetes, Type I and Type II. Type I often known as juvenile diabetes, onset is in childhood and young adults and occurs when the pancreas fails to produce insulin which is the hormone which processes sugar resulting in increased sugar circulating in the blood stream. Type II diabetes, often known as mature onset diabetes, as the name suggests usually happens later in life. Although the pancreas continues to produce insulin the body develops a resistance to it and therefore is unable to metabolize sugar. Although both diseases are controlled differently, Type I requiring injections of insulin and Type II may be controlled by reducing sugar intake (diet) or drugs which help the body to use insulin better. Ultimately the disease causes the same problems to the body, especially if uncontrolled or poorly controlled. There is damage to small blood vessels particularly in feet, hands, eyes, kidneys and heart and damage to nerves. Manifestations in the in the foot are largely three fold, poor circulation, nerve damage and poor healing following injury. Diabetics represent the largest group of lower limb amputees. Complications with the foot due to the manifestations of diabetes can, if not treated promptly can lead to ulceration gangrene.
Foot wise treatment involves assessment of circulation and nerves, education on diabetic foot care, treatment of any presenting issues (nails, callous, corns, ulceration and skin infections). It important to have feet assessed by a podiatrist at least annually, from this assessment it can then be decided whether further regular treatment is required or simply an annual check up.
Fungal infections
Fungal infections are very common in feet and tend to be either in the nails which appears as thickened discoloured and crumbly, or in the skin on the top or bottom of the foot where it can look dry or broken or between the toes when it will look white and may cause the skin to split. There is often an accompanying malodour.
Treatment should aim to treat the cause, which is often moisture and perspiration, while also treating the infection with the appropriate drugs.
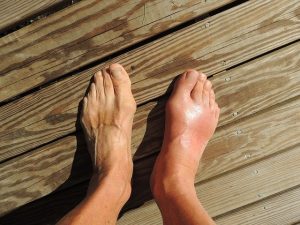
Gout
Is acute joint inflammation caused by a build up of uric acid crystals in the joint. The condition can be so painful that even the bed sheets touching the foot can be too much for some patients.
Initial treatment is aimed at reducing pain anti inflammatory drugs and Laser has proven very effective at settling down the initial pain. In the long term diet and or medication can prevent further out breaks.
Heel Pain
This is a general term used to describe pain in one or both heels; there may be a number of different causes. Probably the most common cause of heel pain is plantar fasciitis (also known as heel spur syndrome) this is covered later in its own section. Other possible causes include loss of fibro fatty padding, bursitis, bony erosions, arthritis, Severs disease and fracture.
Treatment, the most important thing here is correct diagnosis, after that appropriate treatment which may include padding, orthotics, Laser or altering foot ware.
Limb length discrepancy
Many people will have one leg longer than the other often this is why we have one foot larger than the other. Usually the larger foot corresponds to the longer leg where the longer leg has to push down more on the foot causing the arch to lower (pronate) and elongating the foot. Limb length discrepancy may be caused by scoliosis in the back, tilting of the hip, or from one leg being genuinely longer than the other. Often people will go through life with one leg longer than the other and have no problems at all. But symptoms include any problem that is present on one foot and not the other, and can be as diverse as corns and callous, plantar fasciitis, knee problems, bunions, capsulitus, heel pain, metatarsalgia, and even tendonitis.
Once again diagnosis is critical here and appropriate treatment which can include heel raise padding, strapping, orthotics and even onward referral for physiotherapy or orthopaedic specialist.
Metatarsalgia
This is a catch all term for pain in the fore foot (front of the foot just behind the toes) and again there may be one of many causes, Morton’s neuronal, capsulitus, stress fracture and even corn or callous.
Treatment, again diagnosis is all important, then appropriate treatment which may include, laser, padding, strapping, orthotics and or change of foot ware.
Morton’s neuroma
Pain in the fore foot often between the 3rd and 4th metatarsals but may be between the 2nd and 3rd or even the 4th and 5th. The pain radiates forward into the toes and may also be accompanied by numbness and tingling. It is exacerbated by tight foot ware or exercise. It is caused by the nerve being squeezed between the metatarsal heads and getting thickened.
Treatment, the aim here is to reduce the pressure on the nerve, metatarsal domes work well to open the metatarsals up, also laser and orthotics. Surgery may be indicated if conservative measures fail but this in its self is not always effective and may be prone to re occurrence.
Plantar fasciitis
Pain in the heel usually worse on rising in the morning, and improves once the patient “gets going” but can be exacerbated by exercise and is often worse towards the end of the day. This condition is also known as Heel spur, as it was originally thought that the heel spurs which are often seen on x-ray with this condition were the cause of the problem. It is now known that the spur it’s self is not the cause of the problem but rather a symptom of the problem, as surgical removal of spurs rarely improves symptoms. The underlying problem here is inflammation where the plantar fascia attaches to the heel bone caused by increased pull on the plantar fascia. Increased pull may come from sudden increase in activity, over use or change in foot ware.
Treatment is aimed at reducing the pull on the plantar fascia and may include stretches, strapping, changing foot ware, and orthotics and in difficult to treat cases night splints are very effective.
Severs disease
Heel pain associated with activity, this contition affects children and young adults between the ages of about 10-18 years old who are very active in sports. It may affect one or both heels and will be exacerbated by exercise particularly activities that involve running or jumping. The disease usually occurs at about the same time the individual is going through a growth spurt. What is really occurring here is as the bone in the leg grows there is increased pull on the Achilles tendon. As this is attached to the back and under side of the heel it pulls the bone away from the still maturing growth plate causing avascular necrosis and pain. Although the disease is self limiting and the child will eventually grow out of it when they reach maturity it can be very painful and prevent the individual being able to lead a normal active life.
Treatment involves cessation of all activities that cause pain, stretching and orthotics; the use of laser is also useful in speeding the healing process.
Tendonitis
Inflammation of the tendon, this usually results in pain and often swelling. Tendonitis can affect any of the tendons of the foot and may be caused by sports injuries, over use or poor bony alignment.
Treatment will involve resting the area, icing, and laser, in the longer term orthotics may be of use to treat the underlying biomechanical problem.
Ulceration
Ulcers in the foot can be roughly categorised into the following, arterial, venous and neuropathic. Arterial ulcers are due to poor arterial blood supply, this is occurs when the oxygenated blood that is pumped from the heart fails to reach the foot in sufficient quantity to repair a wound or give the skin sufficient nutrition for the skin to be viable. This is caused by hardening and narrowing of the arteries and is often seen in diabetes and peripheral vascular disease (PVD), sometimes also known as peripheral artery disease (PAD). Venous ulceration occurs when the veins (the vessels which take the blood back up to the heart) do not work as well, (varicose veins); ulceration often occurs around the inside of the ankle. Neuropathic ulceration occurs when there is loss of feeling or sensitivity in the foot, damage occurs and is not noticed by the patient leading to ulceration as they continue to walk on the foot. Neuropathic ulceration is common with diabetes. Ulceration occurs when a wound fails to heal or there sufficient pressure on a part of the foot to cause the skin to break down and ulcerate.
Treatment, good wound care is essential here, appropriate dressing and reduction of callous around the wound, reduction of pressure by padding or insoles if the cause is increased pressure to the area. Laser treatment has also proven to be very effective at speeding up heeling. Underlying causes must also be considered improving arterial or venous circulation.
Verruca
Verruca or plantar warts as they are sometimes known as occur when the skin is infected by the verruca virous, human papiloma virous (HPV). Often but not exclucivly seen in children verrucas can be but are not always painful. On the top (dorsum) of the foot they may stick up and look warty in appearance, where as in the bottom of the foot they get pushed into the foot and develop callous over them.
Treatment can be with acid or Laser or may involve freezing them and may well involve several treatments.