Articles

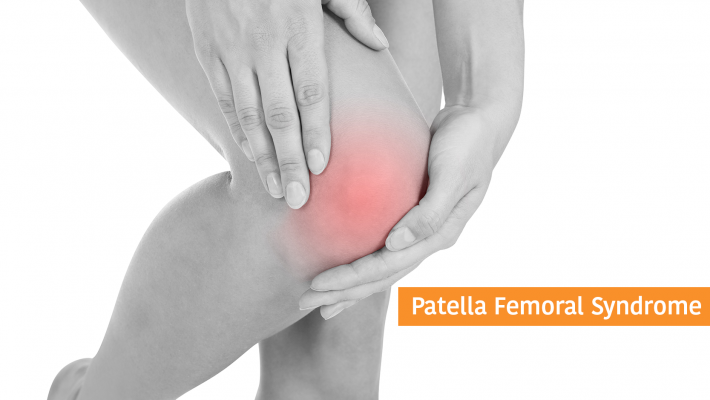
Knee pain and feet
One of the most common knee problems that I see in clinic is Patella Femoral syndrome; also sometimes know as runner’s knee.
The problem causes pain in the front central portion of the knee usually worse when running or walking up or down hill or going up and down stairs (down particularly). Often there can be pain when sitting with knees bent, which is why the condition is also known as theatre goers knee. Pain comes from behind the kneecap (Patella) where it contacts with the thigh bone (femur).
Prolonged excessive shearing forces between the back of the patella and the front of the femur as the patella no longer tracks nicely between the groves formed by the bottom of the femur.
The problem is usually caused by biomechanical dysfunction, over pull of the lateral quadriceps, excessive pronation or supnation (rolling in or rolling out) of the foot. Overuse in sports or activities which are tough on the knee can also lead to patella femoral syndrome, running, jumping, cycling often exacerbated by biomechanical problems.
This results in inflammation, pain and eventually thinning and softening (Chondromalacia) of the articular cartilage behind the patella and on the femur. The condition can also be secondary to fractures, Osteoarthritis and bony tumours, i.e. changes in the bony structure of the knee.
The problem is usually diagnosed on examination and history, although X-ray and MRI can be useful if the diagnosis is not straightforward.
Treatment can involve any or all of the following, controlling excessive biomechanical dysfunction (pronation or supination) of the feet and legs with either strapping or orthotics, quadriceps strengthening, stretching of posterior muscles of the leg and thigh, and sometimes direct treatment to the knee, laser, icing and anti-inflammatory drugs.
Treatment will depend on the severity and duration of the problem and identification of the underlying causes. Prognosis is full recovery, and a return to normal activities once underlying causes are identified and addressed. I think podiatrists are in a unique position the treat this problem as we are able to address the underlying biomechanical problems to resolve the condition. But then I am a bit biased!
Philip Mann Podiatrist/Chiropodist tel: 686 912 307 or www.footpodiatrist.com

Achilles Tendinitis
I seem to be seeing a lot of Achilles Tendinitis in the clinics at the moment. Also known as Achilles tenosynovitis or Achilles tendinopathy.
This condition causes pain in the back of the heel, worse on and after exercise and often particularly painful on rising in the morning. There may be swelling and thickening of the tendon, it may look like a nodule on the back of the tendon.
There are two main presentations of this condition, Noninsertional Achilles Tendinitis and Insertional Achilles Tendinitis, as the names suggest, insertional is in the part of the tendon which attaches into the bone and noninsertional is in the other part. Sometimes the insertional variety is associated with a bony spur formation at the back of the heel (not to be confused with calcaneal heel spur).
So what causes Achilles Tendinitis?
Well as usual there a number of causes it tends to be an overuse type injury, although tight calf muscle in my experience is always present.
Sudden increase in exercise duration or intensity, insufficient stretching before and after exercise, worn shoes and
over pronation where the foot flattens can all contribute.
The condition is common in runners and also sports which involve jumping but can also affect people who are not sporty at all.
The achilles tendon is the largest tendon in the body and it attaches the calf muscle to the back of the heel. It is used to lift the heel and it stores energy each step to help with the following step although very strong it has to have some elasticity.
When someone gets Achilles Tendinitis there is scarring and degradation of the tendon which causes the tendon to become stiff and inflexible. This increases the possibility of rupture. Due to the poor blood supply to achilles it can take a long time to heal. The literature often says six to twelve months although with good treatment I expect it to be a lot quicker.
Treatment of Achilles Tendinitis involves stretching and strengthening, I find Low level Laser works very well as it increases the blood supply to the area and also reduces the pain and swelling.
Rest and cessation of activities which exacerbate the problem, switching to low impact exercise. Ice and anti inflammatories help.
Addressing footwear and controlling the over pronation with strapping or and orthotic. I tend to favor orthotics with a combined heel raise which control pronation and reduce the velocity of the pull on achilles. In severe cases surgical debridement of the tendon may be required.
As with all overuse/sports type injuries there is no single cause to the problem and therefore no single solution and successful treatment is tailored to the individual’s causes and needs.
Philip Mann Podiatrist/Chiropodist 686912307 www.footpodiatrist.com
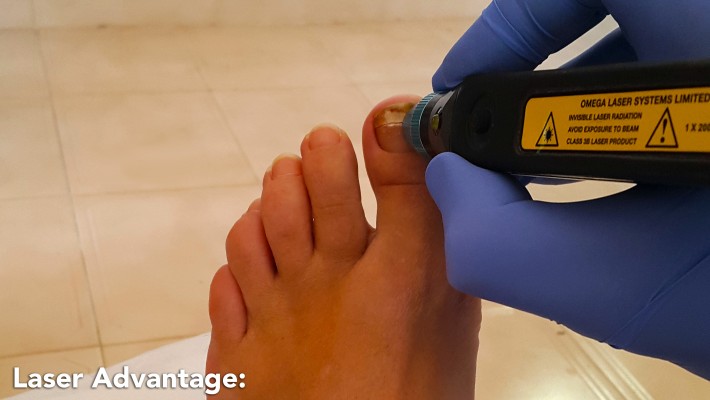
Laser for Fungal Nails
Fungal nails, Onychomycosis affect about between 10% and 40% of the population depending which survey you believe, judging by the amount pharmaceutical companies are prepared to spend on national television advertising there are a lot of people suffering with this condition.
Fungus usually presents as discoloured nails darkened, green/yellow or even white the nail is often crumbly and friable and may or may not be thickened. I am often asked ‘how did I catch this’ and my usual response is damage is the most common cause. The nail is damaged either from acute trauma like kicking the curb, or from more chronic trauma like tight footwear.
The damage to the nail allows the fungus to get into the nail and start eating away at the keratin; the protein nails are made of.
There are other conditions which may look like fungus these include psoriasis and onychomycosis or thickening of the nail. So the first visit is always important to establish that the problem is fungus and not something else.
Before laser the only effective treatments fungal nails were topical paints and lacquers and tablets and although these treatments can be effective they do have their drawbacks as well. Tablets do have potential side effects, liver damage being the one of most concern, but also other less serious problems.
Paints and lacquers work well for fungal nails but require the nail to be cut right back and the treatment takes a long time sometimes more than a year. So people give up or stop before the problem has fully resolved.
The advantage of laser is that it is effective 70/80% success rate, painless no side effects and the patient doesn’t have to do anything themselves.
SO WHAT DOES FUNGAL NAILS TREATMENT INVOLVE?
Well once it is established that it is fungus then treatment starts with cutting the nail back and removing as much infected nail as possible. This has two purposes, one it makes the nails look a whole lot better and two it helps the treatment to be more effective.
Then laser is applied to each affected toe for four to six minutes
THIS IS A PAINLESS PROCESS
Initially four sessions are required and I usually spread them out over a couple of months, as we still have to wait for the nail to grow to see progress. Often only four sessions are required but sometimes I will do a follow up a month or so later and laser again then if required.
If you are interested or require more information about Fungal Nails why not visit my website www.footpodiatrist.com or give me a call on 686912307, if I’m with a patient and do not answer, leave a message and I will call you right back.
Dermatology and Feet
One of the many facets of podiatry is dermatology and if you think about it, feet are covered in skin and nails are just an adaption of skin.
There is now a podiatric speciality known as Podiatric dermatology which has grown out of the fact, that as a podiatrist much of what you do crosses over into dermatology and therefore many podiatrists want to know even more and specialise in this area.
When I go to conferences dermatology lectures are always packed. Many of the routine treatments I am involved in are dermatological in nature, Hyperkeratosis (callous), Heloma durum (corns), Human papiloma virus (verrucas) Onycomycosis (nail fungus) are all dermatological complaints which podiatrists treat every day. There are also the more serious skin conditions that often present in clinic.
Skin cancer is very common in feet as after to hands and faces feet are exposed to the sun probably more than any part of the body. From solar Keratosis sometimes known as sun spots, Squamous cell carcinoma, Basal cell carcinoma and even malignant Melanoma are all commonly seen on feet.
I think I have mentioned before that one of the differential diagnosis for ingrown toenails particularly if they are persistent, is malignant Melanoma. Obviously with skin cancers it is not a podiatrist’s role to treat them and swift referral especially in the case of suspected Melanoma to a Dermatologist is essential.
But malignancy aside, there are still many skin conditions of the feet that podiatrists treat very well. Cracked heels are very treatable with debridement and advice on the correct emollients. Often cracked or split heels are a symptom of psoriasis and psoriasis has other manifestations in the feet one of which is psoriatic nails. These often look just like fungal nails and although the psoriasis in nails cannot be eliminated it can be managed very well by reducing the nail bulk and improving appearance.
Athlete’s foot which is really a fungal infection is a very common presentation in clinic in its many forms. Even bacterial infections like Pitted Keratolysis where white holes are seen in the bottom of the feet especially when wet are very treatable in clinic.
There are too many skin conditions seen in feet to mention them all, but the above are a few which are commonly seen.

Permanent Solutions to Ingrown Toenails
A PERMANENT SOLUTION TO INGROWN TOENAILS
Ingrown toenails are one of the most painful conditions that I treat in my clinics, but the treatment itself is virtually painless.
It always surprises me when meet patients who have been having an ingrown toenail treated for a long time sometimes many years and they have not been offered a permanent solution to the problem.
It makes me suspicious that either the person who is treating them wants them to keep coming back to have the same problem treated, or that they are not qualified to do the surgery and therefore working illegally.
In order to work in Spain as a podiatrist/chiropodist you must be able to to do basic surgery under local anesthetic. But I am getting a bit ahead of myself.
What is an ingrown toenail?
Well it’s where part of the edge or front of the nail pushes into the skin causing the toe to become sore swollen and inflamed. The condition occurs mainly on the 1st toe and is really very much like having a splinter. It is a foreign body in the skin which needs removing. Just like a splinter once removed the pain disappears and the area settles down and returns to normal.
Sometimes that is all that is needed, if the nail was cut badly taking away that sharp or rough edge is all that is required a little careful cutting by someone who knows what they are doing and is at the right end of the body to see what they are doing.
Unfortunately often the problem re occurs this is usually because the nail has become a little curved. This is when a permanent solution should at least be offered.
This is how it works in my clinics, if you present with an ingrown toenail, initially I will remove the bit and make you comfortable on the first visit, I will talk about surgery as an option but this option is up to the patient. My advice is usually something like. If this a problem once or twice a year come back and I will just cut a little bit away.
But if this keeps being a problem every month or two then you should consider surgery as it is a permanent solution. This is elective surgery so you decide if you want it and when it is convenient to have the procedure. I am happy to keep cutting a little bit off if that is what the patient wants. Some people are happy with that others may not be suitable for surgery due to problems with health, circulation and diabetes are considerations.
Ninety percent of the time I do not remove the whole nail but just a strip all the way down the side so after you still have a nail and it doesn’t really look much different except I have removed the bit that curved into the skin.
Although I do not like to say it is a totally painless procedure, the vast majority of people and I do a lot of this on children, say it is virtually pain free. The anesthetic is put in at the base of the toe where it joins the foot away from the sore bit and this makes the whole toe numb. Once the part of nail is removed the area is treated with phenol to prevent the nail growing back. I allow people to swim, shower and get on with life following the surgery but most people will want to be in an open shoe for at least a week following the procedure.
If you have been suffering for a long time it is really something to consider and nothing to fear.
Philip Mann Podiatrist Chiropodist 686 912 307
Who would be a Podiatrist?
Without doubt the question I get asked most at work is why would you want to be a podiatrist and look at smelly feet all day?
The question is often a lightly veiled way of saying do you have a foot fetish or something and some people even ask this outright.
This is usually followed by: Have you always wanted to do this since you were at school?
This normally happens about half way through the first consultation. They have already told me what the nature of the problem is I have taken a medical history and asked them questions about their symptoms and I am probably doing some kind of treatment.
I suppose the question is fair enough; on the face of it looking at feet all day is not the most glamorous way to spend your day.
Well in reverse order this is what I normally tell people. I haven’t always wanted to do this. When I left school I trained as a dental technician and made false teeth until I was about in my mid twenty’s.
No I do not have a foot fetish. As to why? Well I really enjoy my work, most people I see come to me in pain and go away feeling better. So there is lots of job satisfaction and people are usually pleased to see me.
There is also a tremendous amount of variation in what I do each day, from nail cutting and corns to looking at people’s biomechanics and gait analysis, minor surgery under local anaesthetic for removal of part of or a whole toe nails, assessment and treatment of diabetic foot problems, wound care, children’s foot problems, sports injuries, treatment of verrucas to name but a few.
Also there is quite a lot of problem solving in my work, clients will come in with a pain in their foot there may be very little to see in the way of obvious signs like swelling and redness and I have to diagnose and treat the problem.
Sometimes a treatment that works for one individual will not be as successful for another with the same condition so an alternative solution tailored to the individual must be found. This all makes my work interesting and rewarding.
Then of course I get to spend at least half an hour a time with my patients and we get to chat, so I get to know people and people are generally interesting. And I know I am not alone, most of my collages are enthusiastic and passionate about what they do. If I go to a conference podiatrists are always keen to learn new techniques and share experience and knowledge.
Don’t get me wrong I don’t get up every morning and leap out of bed and go” great feet again today!” but I do consider myself very lucky to have a job I really enjoy.

Role of a podiatrist
The term Podiatrist means foot specialist, someone who will manage all areas of foot care from simple nail cutting and treatment of corns and callous to assessment and treatment of Diabetic foot problems, minor surgery under local anaesthetic and sports injuries.
One of one of the questions that podiatrists get asked most is “how can you do this job looking at smelly feet all day?” well there is a great deal of variation; during the course of a clinical session they may find them self treating sports injuries, ingrown toe nails, corns and callous, Painful bunions, Heel pain and plantar fasciitis, diabetic ulcers , infections of the skin and nails, Verrucas (planter warts), children’s foot problems, or doing gait analysis, biomechanical assessment and prescribing orthotics. Generally speaking patients arrive in pain or discomfort and go home feeling better so there is a lot of satisfaction although maybe not much glamour.
Most first time consultations will start with a medical history as the feet cannot be treated in isolation and many systemic illnesses can affect the feet and vice versa. This is usually followed by examination and then diagnosis. Diagnosis is crucial; if this is wrong the treatment is bound to fail. Once a diagnosis is made this is carefully explained to the patient and or their guardian and treatment options discussed. A treatment plan can then be made based on informed choices from patient and practitioner.
Many of the problems encountered in the foot have an underlying biomechanical problem. This means that the problem is due to the way the feet and legs function, feet may “flatten out “or the arch may be too high. In turn this may cause increased pressure or stress on a particular part of the foot or leg leading to pain and dysfunction. A podiatrist can assess the alignment problem and prescribe the appropriate orthotic foot support to go into the shoe, as well as address any problems with muscle weakness or imbalance.
Podiatrists play a crucial role in diabetic foot care. Diabetes can have significant impact on the health of the feet and sadly diabetics represent the largest group of lower limb amputees. Diabetes can damage blood vessels and nerves in the feet and affect healing in the feet. But complications are avoidable with good education, diabetic control and assessment of diabetic patient’s feet. This usually involves looking at blood flow using Doppler ultrasound and assessment of any nerve damage in the foot. Advice on foot ware and care will be given. Prevention is definitely the key here and diabetic feet should not be ignored.
In our journey through life it is the feet that do the hard work but are often sadly neglected, so look after them make that appointment to see the podiatrist today.
Heel Pain
Heel pain is one of the most common problems that I see in the clinic and can be a very debilitating condition
Probably the most common type of heel pain is Plantar Fasciitis or as it is sometimes known as Calcaneal heel spur syndrome. Although heel spurs are often visible on X-ray this is not always diagnostic as they are also often seen on the non symptomatic foot too, and diagnosis is usually on history and symptoms. This condition is characterized by increased pain with the first steps in the morning or when standing after a prolonged period of sitting. It can be in one or both feet. There are many treatments available for this condition depending on the severity of the condition the length of time the individual has had the problem and level of activity, and can vary from stretching and strapping to orthotics and even night splints.
Achilles tendonitis is usually a sports injury or can be caused by over use or even foot ware. Pain is often worse on rising in the morning and exacerbated by activity. Treatment, laser treatment is very effective here and stretching is important also altering foot ware can also help.
Hagland’s deformity or Pump bumps as they are sometimes known are boney lumps at the back of the heel on the outside. Caused by the foot rubbing on foot ware the body attempts to protect the area laying down more bone. Sometimes there is an associated fluid filled sac called a bursa associated with this condition. The area can become inflamed and very sore in shoes. Treatment, controlling the motion of the foot, padding and laser work well, although surgical intervention is sometimes called for.
Bursa can also be a problem behind the Achilles tendon and in the fat pad of the heel. If these bursa become inflamed they can be painful on activity. Once again laser can be very good here as can padding or an accommodating insole.
Sever’s disease is a heel condition only seen in children and adolescents, eight to about 16 years old and is quite common. Usually seen in very sporty individuals, pain is exacerbated by exercise and often is only present when running or jumping. Often Sever’s coincides with a grown spurt as the leg bone grows and the Achilles tendon pulls on the heel bone pulling the growth plate of the bone away and causing localized avascular necrosis with resultant pain on exercise. Orthotics and stretching work very well here enabling the child recover fully and return to the sports they enjoy.
There are many conditions which cause heel pain from tumors, fractures to simple splits. I have just covered a few examples here.
Diabetic foot care
Why Diabetic foot care is important
With the incidence of diabetes on the increase in the western world, the importance of foot care for diabetics has never been more important. Sadly diabetics represent the biggest group of lower limb amputees even greater than that of road traffic accidents. But it is not all bad news diabetic amputations are avoidable and in this article we will look at the causes and how to avoid problems leading to amputation.
Diabetes is an increase in circulating blood sugar levels; there are two types of Diabetes, Type I and Type II. Type I often known as juvenile diabetes the onset is in childhood and young adults Type II diabetes, usually known as mature onset diabetes, as the name suggests mainly starts later in life. Both diseases are controlled differently, Type I requiring injections of insulin and Type II may be controlled by reducing sugar intake (diet) or drugs which help the body to use insulin better. Type II may eventually require the use or insulin too. Ultimately the disease causes the same problems to the body, especially if uncontrolled or poorly controlled. There is damage to small blood vessels particularly in feet, hands, eyes, kidneys and heart and damage to nerves.
Manifestations in the foot are largely three fold, poor circulation, nerve damage and poor healing following injury. But just because you are diabetic it does not mean that you will automatically have all of the following problems. If diabetes is well controlled it has a minimal effect on the body so controlling your blood sugar levels is very important.
Circulation can be effected by accelerating arthrosclerosis, the hardening of the arteries; this makes it more difficult for the blood to get to where it needs to go. If the blood can’t get down there in sufficient quantity or quality, when an injury occurs it may be slow to heal or even ulcerate. If the ulceration is not treated it can get infected and if that infection is not treated it can turn to gangrene which would mean amputation of the affected toe, foot or even leg. But as you can see there are many chances for intervention, from treating the original injury to treating the ulceration to treating the infection. Obviously it is better to treat the original injury early and avoid the complications of ulceration and infection.
Nerve damage or neuropathy can occur with diabetes. This can lead to loss of feeling particularly pain sensation in the feet. The problem here is the individual may not be aware that there is loss of feeling and if there is an injury may not seek care promptly. This increases the dangers of the above complications. Over the years my diabetic patients have been extremely inventive when it comes to damaging their feet without realizing it. From simple things like blisters and sun burn to scalding feet in a hot bath to the extreme cases of walking round with a nail through their shoe into the foot, all treatable but also all avoidable.
Poor healing in diabetic feet means that injuries are often slow to heal so wounds stay open longer increasing the chances of getting infected and infections love sugar. The higher the blood sugar the more rapidly the infection can take hold.
So what can we do to avoid these problems? Well, plenty. Good diabetic control means less damage and less problems. Inspect the feet daily make sure there are no injuries or changes in colour, inflammation or pain, if need be look at the bottom of the feet in a mirror if you have problems getting down there. Don’t walk bare foot it’s just asking for trouble. Wash the feet daily and dry carefully between toes and apply moisturiser to any dry areas, but not between the toes. Have feet measured when buying shoes and always check inside shoe before putting it on for stones or other foreign bodies. Visit a Podiatrist, well I would say that, but foot assessment by a podiatrist is important, circulation can be checked with Doppler and neuropathy measured then tailored advice given as well as routine care of nails corns and callous and even ulcers. If you have a foot problem don’t ignore it or try to self treat or self diagnose. Unfortunately there are too many amputees who put off seeking medical attention worried as they had heard about diabetics losing limbs, so that by the time they actually do seek care it is too late. Early intervention and treatment is the key to avoiding serious foot problems and having peace of mind.